






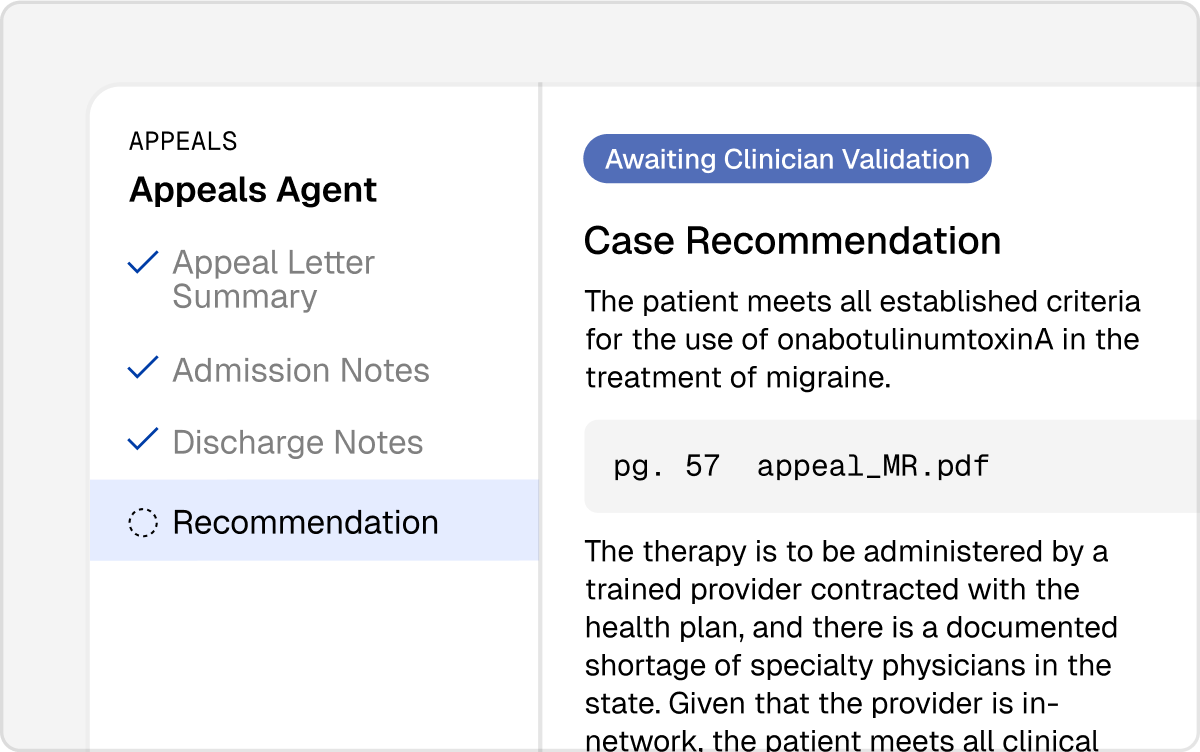
Extract key clinical insights from complex medical records to support stronger, more defensible appeals without manual chart review.
Automatically route straightforward cases to resolution without clinician involvement, so your team's time is reserved for complex appeals that require human judgment.
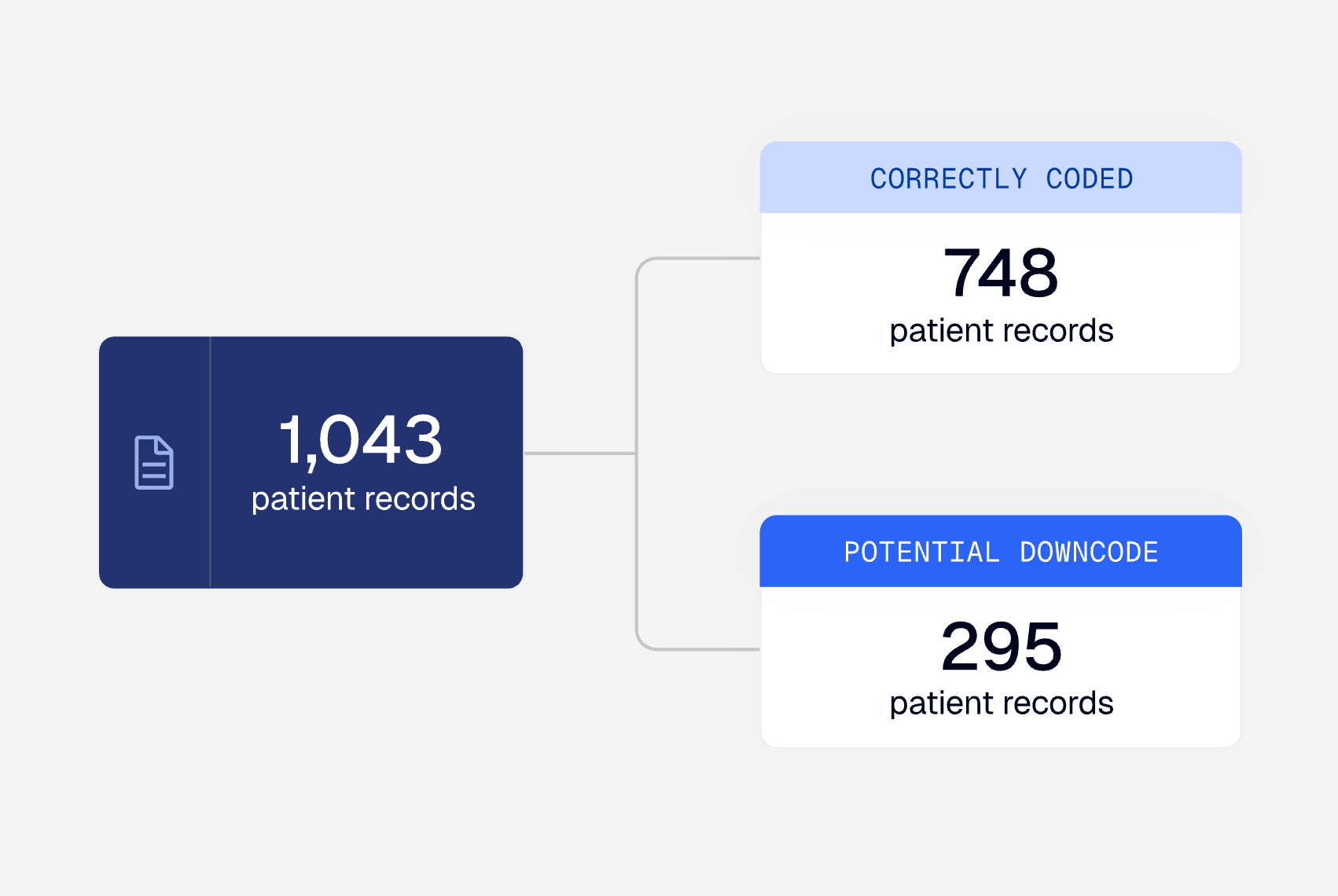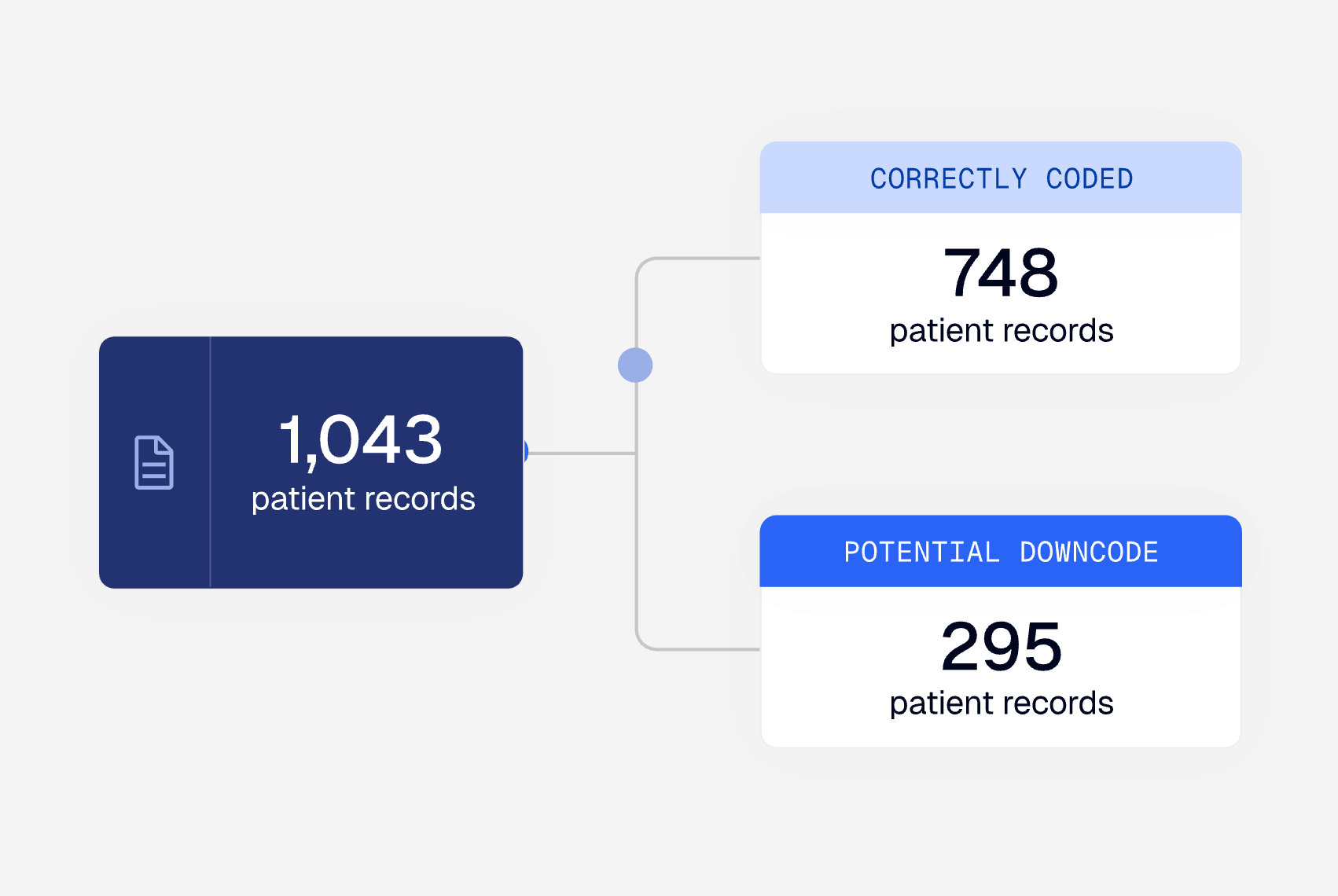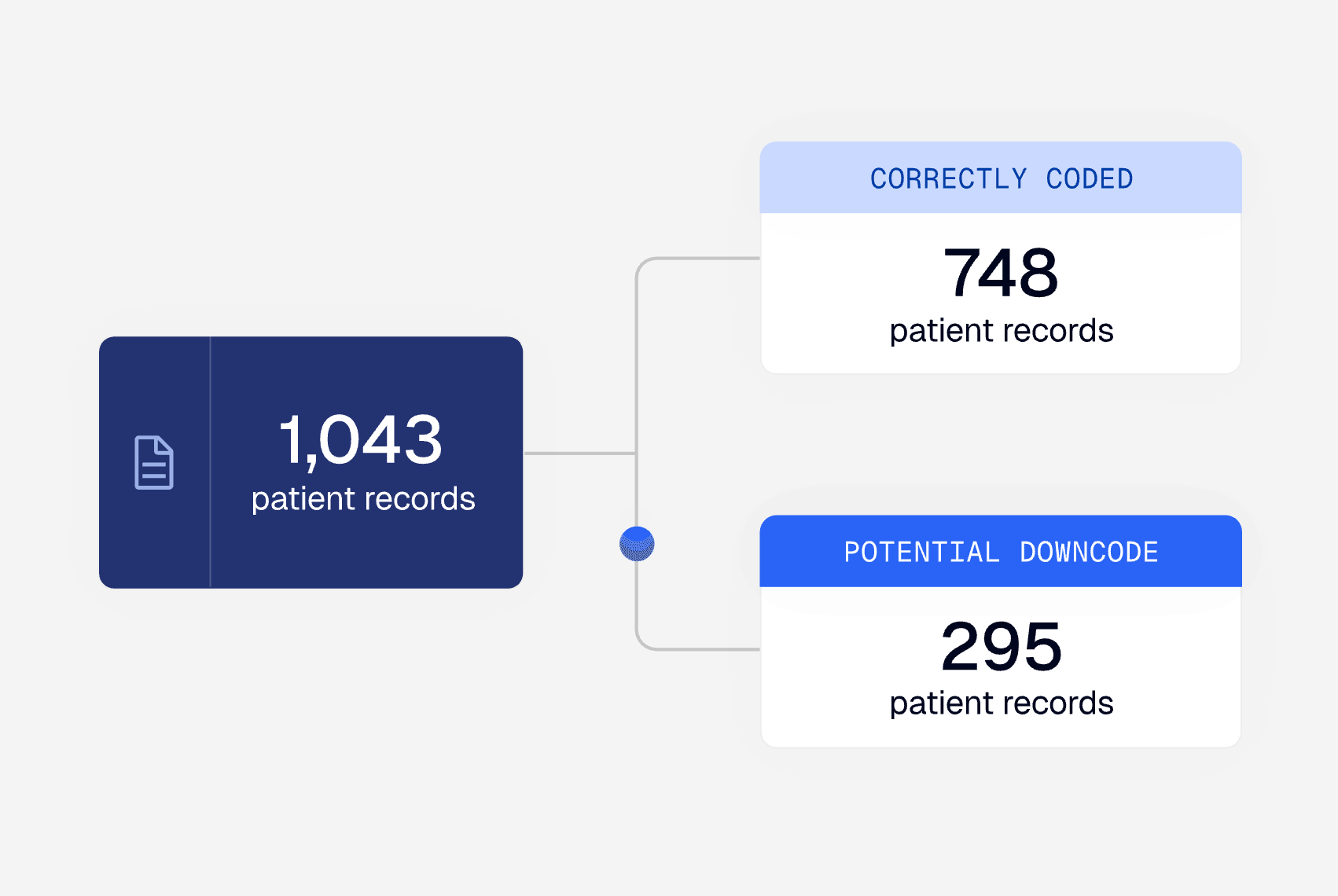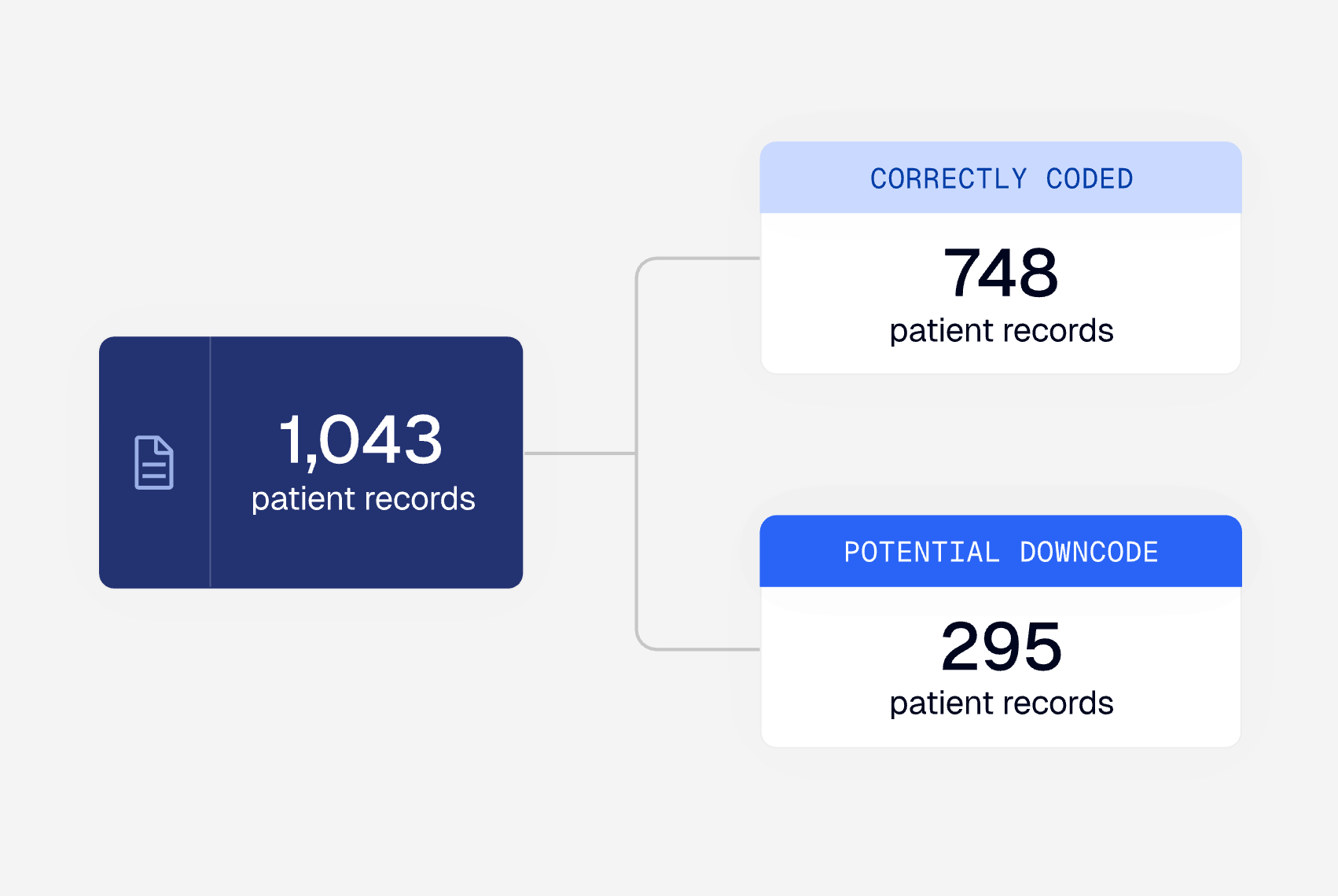
Automatically analyze and rank denials based on financial impact and likelihood of overturn, using clinical reasoning against medical records, policy guidelines, and relevant criteria to surface the most actionable recommendations for your team.



Traditional appeals management vendors rely on slow, expensive manual clinical review, inconsistent determinations driven by reviewer variability, and reactive workflows that struggle to keep pace with rising appeal volumes. We take a different approach, using purpose-built AI agents configured to your internal policies and documentation standards to both reduce appeals at the source and resolve the rest faster, supporting pre- and post-service, emergency service, level of care, and DRG and coding appeals.
By automating the clinical review and letter drafting process, Alaffia increases throughput and frees clinical staff to focus on the most complex cases that require human judgment. Every recommendation is backed by a clear clinical rationale with traceable source citations, resulting in faster turnaround times and more consistent and defensible determinations, so your team can handle more appeals without added headcount.
Our managed services and SaaS solutions support appeals, utilization management, and payment integrity by giving teams the clinical context and operational intelligencethey need to work faster and with greater accuracy.
By automating the intake, summarization, and cross-referencing of medical records against clinical criteria and coding guidelines, we dramatically increase the throughput and accuracy of clinical reviewers across all these program areas, driving consistently better outcomes across the entire claims lifecycle.
Our platform integrates seamlessly with existing claims management systems, EHR data feeds, and clinical criteria tools. It does not require health plans to replace existing infrastructure.
Yes. Our solutions support clinical workflows across the entire claims lifecycle.
We’ve achieved a 97%+ accuracy rate across all client implementations.
We get up and running in just 30 days from contract to production, with immediate ROI. Integration into your current systems is seamless, with no disruption to your operations or changes to your workflows.
Alaffia doesn’t replace your clinical team — it makes them even more valuable. Our AI agents increase throughput 20x, routing clear approvals for immediate processing while flagging complex cases. That frees up your clinicians to work at the top of their license, focusing their time and expertise where it matters most instead of dealing with routine cases.
As for vendors: we support clinical workflows across the entire claims lifecycle, whereas most vendors are point solutions that only handle specific workflows or sub-problems. Our unique hybrid engagements are tailored to meet you where you are, so we are capable of replacing multiple vendors if that’s what makes sense for your plan.
Privacy, security, and compliance are built into every layer of our solutions. We adhere to SOC-II Type II, HIPAA, and HITRUST security standards, and we establish and implement custom governance controls. All data stored within our platform is encrypted in transit and at rest, with 256-bit encryption to protect confidentiality and privacy.
Yes. Building alongside your team, we configure our software to meet any clinical needs you have, with your plan’s specific data, policies, and processes integrated into our AI platform to create bespoke workflows and outputs. Our AI agent will mimic your audit process and follow your decision tree on the way to making recommendations.